Throughout millennia, humans have used alcohol. An approximately 13,000-year-old brewery in a burial site in a cave in the Middle East provides the earliest evidence of human consumption of alcohol to date. There, scientists discovered stone mortars carved into the cave floor containing traces of a wheat- and barley-based alcohol. They theorized that these early humans used the beer in ritual feasts to honor their dead. Other scientists propose that the human desire for alcohol may have spurred the development of agriculture. Later evidence of alcohol consumption, such as during the Chin (Jin) dynasty in China, indicated that humans found multiple uses for it, including in medicine and in social and spiritual activities. The idea of alcohol as beneficial to health persists today in some of our current drinking toasts, such as “To your health!”
However, in January 2025, former U.S. Surgeon General Dr. Vivek Murthy issued Alcohol and Cancer Risk. It contains an alarming message: “This advisory highlights alcohol use as a leading preventable cause of cancer in the United States, contributing to nearly 100,000 cancer cases and 20,000 cancer deaths each year.”

The advisory comes on the heels of similar statements from the World Health Organization (WHO) and represents a meta-analysis of the most recent and historical data centered on three aspects of alcohol use: (1) consumption rates; (2) incidence of attributable cancer cases and cancer deaths; and (3) lack of public awareness of cancer risk. Considering this body of evidence, the surgeon general calls out alcohol use as the third preventable cause of cancer, after tobacco use and obesity, in the United States. The advisory sounds the alarm particularly for women, who bear the heaviest burden of risk, with alcohol-attributed breast cancer contributing to 16% of the 270,000 breast cancer cases in 2019.
The surgeon general’s advisory recommends several actions, including a call for Congress to add cancer warnings to alcohol labels, similar to the health-hazard labels added to cigarette packaging in 1965, about a decade after the American Cancer Society confirmed the causal link between cigarette smoke and lung cancer. Warning labels about alcohol’s risks to pregnancy and driving appeared in1988 but have not been updated since.
The 40-year gap
Several studies in the 1980s showed a causal link between alcohol use and cancer, leading the WHO’s International Agency for Research on Cancer to classify alcohol as a Group 1 human carcinogen in 1988. Several U.S. agencies, such as the CDC and the 2016 Surgeon General’s Report, concurred. In January 2023, the WHO declared that no level of alcohol consumption was safe for human health, adding, “Currently available evidence cannot indicate the existence of a threshold at which the carcinogenic effects of alcohol ‘switch on’ and start to manifest in the human body.”
Why did the U.S. Surgeon General neglect to sound an alarm by providing an advisory about alcohol’s dangers for almost 40 years, and why has the cancer risk of alcohol consumption escaped public attention? The answer lies partly in the difficulty of conducting meta-analyses of studies comprising heterogeneous methodologies and data sets. Other contributors to this lack of widespread public knowledge relate, perhaps, to reliance on observational data combined with wishful thinking and deft marketing.
A 1992 Lancet epidemiology paper and later studies reported on the “French Paradox” between wine and high fat consumption and increased cardiovascular health in the French. Within a year of the news, red wine consumption in the United States nearly doubled, and merchants began to promote red wine as a health food. Scientists continue to try to solve the French Paradox, including in in vitro and in vivo studies of resveratrol, a polyphenol antioxidant thought to be the protective ingredient in red wine, but they have never established a causal link between red wine consumption and increased cardiovascular health.
Consumption and Cancer
Data on the rate of alcohol consumption in the advisory comes from the Alcohol Research Group’s 2020 survey on U.S. drinking norms. It reveals that 72% of U.S. adults consume one or more alcoholic drinks per week, with 85% of women and 88% of men drinking within moderate limits suggested by the Dietary Guidelines for Americans: one alcoholic drink daily for women and no more than two drinks daily for men (Figure 1).
More recently, we saw evidence of how societal crises, such as the COVID-19 pandemic, induced social isolation and economic challenges that encouraged alcohol and other substance use. In a 2021 paper, Lee et al. reported a 34% increase in total sales of alcohol to over 70,000 U.S. households from April to June 2021.
Data on the incidence of cancer cases/deaths attributable to alcohol spans from recent historical evidence to the most contemporary. In 2024, a paper by Islami et al. revealed that cigarette smoking, excess body weight, and alcohol consumption contributed to 28.5%, 7.3%, and 4.1% of all cancer deaths in 2019. Also in 2024, based on the Center for Disease Control and Prevention’s 2020–2021 survey, Esser et al. reported that 16,800 deaths (83% of the total 20,216 annual cancer deaths attributed to alcohol, which represented 2.8% of all cancer deaths) would have been prevented if drinkers had consumed alcohol at levels within the dietary guidelines. Consumers, however, should not rely on the “safety” of the dietary guidelines; while the advisory notes that cancer risk proportionally relates to the level of alcohol consumption, several studies show that for some cancers, like breast and throat, the risk of cancer may start to increase at around one or fewer drinks per day. Further, it notes a counterfactual from the Esser et al. paper: 17% of people who die from alcohol-attributed cancer actually follow the drinking guidelines.
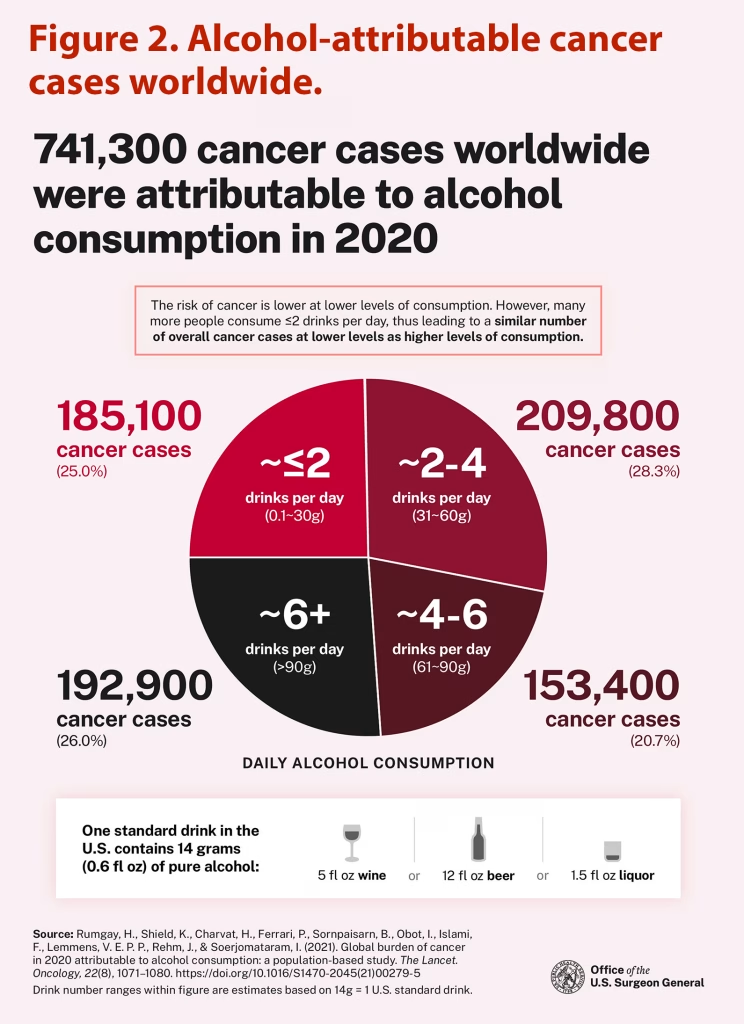
In addition, no one should think of alcohol cancer risk as only an American problem. The advisory cites global data reported in a 2021 paper by Rumgay et al. on the burden of over 740,000 cases of cancer attributable to alcohol (Figure 2).
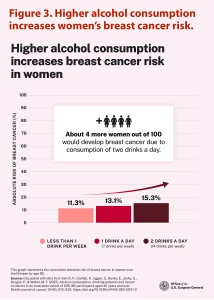
Further complicating risk assessment is that alcohol-attributed cancer varies among organ systems and genders, as for example in Rumgay et al.’s paper, which shows the highest incidences in esophageal (26% of cases), liver (21%), and breast (13%) cancers; and in Esser et al.’s paper, which indicates that 60% of alcohol-related cancer deaths occurred in women in 2020–2021. Because people often underreport their alcohol use, Esser et al. adjusted their survey data to per capita alcohol sales in their 2024 paper. Risk statistics in the advisory include those by Sarich et al., which projected the cumulative absolute risk of breast cancer (from 11.3 to 15.3%) for women drinking at levels below, within, and above the recommended daily guidelines over a lifespan of 80 years (Figure 3). These statistics took their basis from an Australian cohort in 2021. In contrast Sarich et al. reported that alcohol consumption in men contributed mostly to liver (33%) and colorectal (21%) cancers, among their cancer-related deaths.
In light of increasing evidence that alcohol consumption increases cancer risk, scientists are currently reviewing the U.S. Dietary Guidelines and expect to release an update later this year.
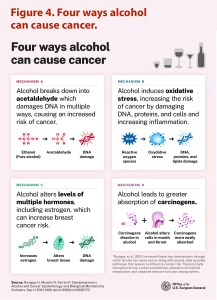
The Surgeon General’s advisory visualizes four ways (Rumgay et al. 2021) that alcohol may cause cancer, including its impact on hormones (Figure 4). Notably for women, alcohol increases levels of estrogen, which can promote breast cancer, particularly in estrogen-receptorpositive cells. Other mechanisms include damage to DNA, oxidative stress, and greater absorption of carcinogens.
Recommendations

More public awareness is needed. The American Institute for Cancer Research’s 2019 Cancer Risk Awareness Survey revealed that although most American adults recognize the increased cancer risk from radiation, tobacco, and asbestos (91–81%), and slightly more than half recognize the cancer risk from obesity (53%), less than half, or 45%, recognize that alcohol contributes to cancer risk (Figure 5). Public awareness of the cancer risk of alcohol has not improved even as documentation of the causal link between alcohol consumption and cancer risk has strengthened.
In a poignant case of the need to build public awareness of this issue, Kari Vandenberg-Bastian, a health-care professional, became aware of the cancer risk of alcohol only after she got a diagnosis of stage 4 breast cancer at age 37 in 2023. Recalling her drinking as a regular part of her professional and social activities in a May 2025 article in the Wall Street Journal, she said, “You know it is bad for your liver, but breast cancer? People deserve access to clear and unbiased information, and I am in awe that I didn’t have that, even as a nurse.”
Not everyone seems ready to issue the last call for alcohol. Because of the complex nature of the data and the lack of randomized studies on moderate drinking, Mukamal and Rimm, who together have 60 years of experience in studying the health effects of alcohol, suggest that we put the brakes on making broad assumptions. In their essay “Is alcohol good or bad for you? Yes.” in Harvard Public Health, they write, “To get a clearer picture of the health effects of alcohol, researchers and journalists must be far more attuned to the nuances of this highly complex issue.”
They continue, “One major challenge in this field is the lack of large, long-term, high-quality studies. Moderate alcohol consumption has been studied in dozens of randomized controlled trials, but those trials have never tracked more than about 200 people for more than two years. Longer and larger experimental trials have been used to test full diets, like the Mediterranean diet, and are routinely conducted to test new pharmaceuticals (or new uses for existing medications), but they’ve never been done to analyze alcohol consumption.”
The measures the U.S. surgeon general proposes, such as warning labels on containers, are warranted in light of compelling evidence of the lack of public awareness of the cancer risk of alcohol consumption, especially the relationship between alcohol and breast cancer in women. However, because of the complexity of the data and its interpretation, scientists must continue to explore the effects of alcoholic substances, which have been at the heart of human interactions for millennia.
 Patricia Soochan was a senior program strategist in Data Science, Research, and Analysis in the Howard Hughes Medical Institute’s former Center for the Advancement of Science Leadership and Culture. In her role, she collaborated with the center’s programs to capture, analyze, synthesize, and communicate program-level data to promote organizational effectiveness and evaluation. Previously she shared lead responsibility for the development and execution of the Inclusive Excellence (IE1&2) initiative and had lead responsibility for science education grants provided to primarily undergraduate institutions, a precursor of IE. She is a member of the Change Leaders Working Group in the Accelerating Systemic Change Network and is a contributing writer for AWIS Magazine and The Nucleus. Prior to joining HHMI, she was a science assistant at the National Science Foundation, a science writer for a consultant to the National Cancer Institute, and a research and development scientist at Life Technologies. She received her BS and MS degrees in biology from George Washington University.
Patricia Soochan was a senior program strategist in Data Science, Research, and Analysis in the Howard Hughes Medical Institute’s former Center for the Advancement of Science Leadership and Culture. In her role, she collaborated with the center’s programs to capture, analyze, synthesize, and communicate program-level data to promote organizational effectiveness and evaluation. Previously she shared lead responsibility for the development and execution of the Inclusive Excellence (IE1&2) initiative and had lead responsibility for science education grants provided to primarily undergraduate institutions, a precursor of IE. She is a member of the Change Leaders Working Group in the Accelerating Systemic Change Network and is a contributing writer for AWIS Magazine and The Nucleus. Prior to joining HHMI, she was a science assistant at the National Science Foundation, a science writer for a consultant to the National Cancer Institute, and a research and development scientist at Life Technologies. She received her BS and MS degrees in biology from George Washington University.
This article was originally published in AWIS Magazine. Join AWIS to access the full issue of AWIS Magazine and more member benefits.

